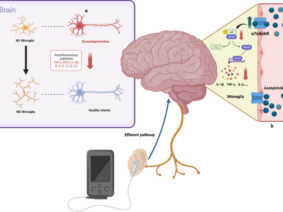
Major Depressive Disorder (MDD) and anxiety are prevalent mental health conditions that continue to challenge the medical community. In recent years, Auricular Vagus Nerve Stimulation (AVNS) has emerged as a promising non-invasive approach for their treatment. AVNS involves the stimulation of the vagus nerve through the auricle of the ear, offering potential advantages over traditional treatments. As research in this field advances, understanding the immediate effects of AVNS on brain networks becomes crucial for optimizing its efficacy and applicability.
Immediate Modulatory Effects on Brain Networks:
A recent research article by Jifei Sun et al. sheds light on AVNS’s immediate modulatory effects on the brain networks of individuals with MDD. The study reveals that AVNS has an immediate impact on the Default Mode Network (DMN) and Cognitive Control Network (CCN). These functional networks play crucial roles in regulating emotional processing and cognitive functions, making them key targets for MDD and anxiety treatment.
The study suggests that targeting these networks through AVNS may provide instant relief to patients, indicating its potential as an effective therapy for those in urgent need of relief from their symptoms. Furthermore, the non-invasive nature of AVNS circumvents the need for surgical procedures, reducing risks and discomfort associated with more invasive treatments.
Advantages of Auricular Vagus Nerve Stimulation:
AVNS offers several advantages over traditional treatment options for MDD and anxiety. By being non-invasive, AVNS avoids surgical procedures and associated risks, making it a safer alternative for patients. Additionally, AVNS sessions are relatively short and can be performed in the comfort of one’s home, promoting convenience and accessibility for individuals seeking relief.
Meta-Analysis on Vagus Nerve Stimulation Therapy:
In a systematic review and meta-analysis by Uliana M. Bottomley et al., the impact of Vagus Nerve Stimulation (VNS) therapy in patients with treatment-resistant depression (TRD) was assessed. The analysis included all outcomes of longer-term adjunctive VNS in various studies, irrespective of TRD severity, comparing them where feasible with treatment-as-usual (TAU). The meta-analysis demonstrated that antidepressant benefits improved up to 24 months, and safety issues were minimal. Despite limitations in the evidence base, VNS+TAU outcomes suggest promising results for this hard-to-treat chronic population.
The combination of findings from Jifei Sun et al.’s research on AVNS and Uliana M. Bottomley et al.’s meta-analysis on VNS provides valuable insights into the potential of non-invasive vagus nerve stimulation therapies for MDD and anxiety. AVNS shows promise as a revolutionary approach to alleviate the burdens of these mental health conditions and offers rapid relief to those in need. As research in this area continues to advance, the future holds the promise of even more effective and personalized treatments for depression and anxiety. However, it is essential to consult with healthcare professionals to determine individual suitability for these therapies. With the increasing prevalence of depression and anxiety globally, alternative therapies like AVNS and VNS represent hope for enhancing mental well-being on a broader scale.
References:
- Jifei Sun, Chunlei Guo, Yue Ma, Shanshan Gao, Yi Luo, Qingyan Chen, Yang Hong, Xiaobing Hou, Xue Xiao, Xue Yu, Peijing Rong, Jiliang Fang, Immediate modulatory effects of transcutaneous auricular vagus nerve stimulation on the resting state of major depressive disorder, Journal of Affective Disorders, Volume 325, 2023, Pages 513-521, ISSN 0165-0327, https://doi.org/10.1016/j.jad.2023.01.035.(https://www.sciencedirect.com/science/article/pii/S0165032723000472)
- Juliana M. Bottomley, Corinne LeReun, Alex Diamantopoulos, Stephen Mitchell, Bradley N. Gaynes,
Vagus nerve stimulation (VNS) therapy in patients with treatment resistant depression: A systematic review and meta-analysis, Comprehensive Psychiatry, Volume 98, 2020, 152156, SSN 0010-440X, https://doi.org/10.1016/j.comppsych.2019.152156.
(https://www.sciencedirect.com/science/article/pii/S0010440X19300793)